The use of technology is unavoidable to keep healthcare affordable and accessible, but its implementation must go hand in hand with respect for patient values, says trauma surgeon Maarten van der Elst. He has been appointed to TU Delft’s Reinier de Graaf chair for the coming five years and is holding his inaugural address on 4 March.
“The healthcare sector is literally out of money, so if we don’t make it more efficient and cheaper soon, we will end up creating a real social divide, with enormous waiting lists and debates about whether procedures like cataract or hip operations are really necessary,” says trauma surgeon and professor Maarten van der Elst. “The population is ageing and people live longer with chronic disorders like cardiovascular diseases, HIV and diabetes. This means there are more and more people who need care, but less and fewer people who can or want to provide it. With the help of technology, we can keep healthcare affordable and accessible to all.”
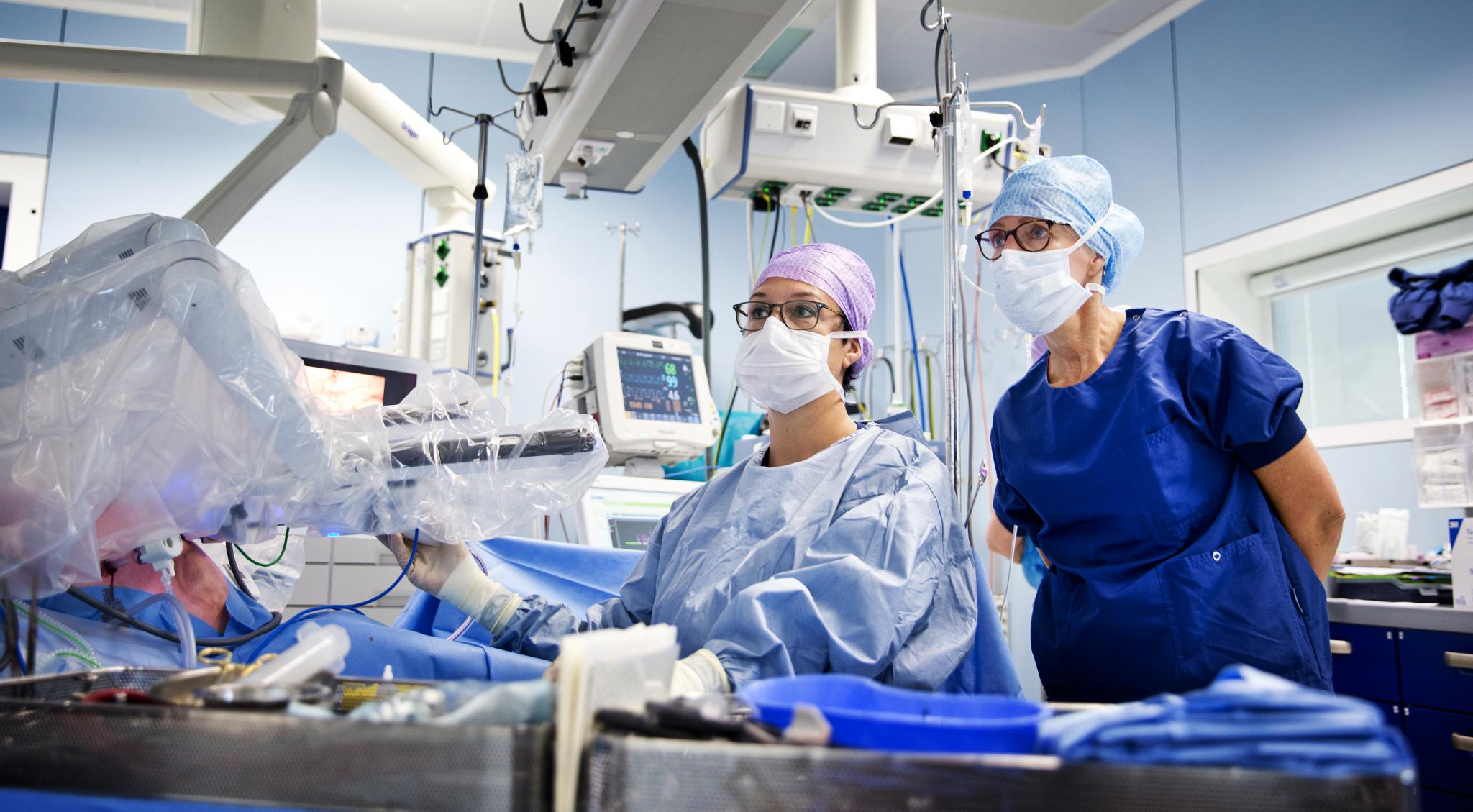
 “When you find yourself on such an operating table, you fully realise that you are surrendering yourself not only to doctors and nurses but also to all the equipment they use. You can only hope that the staff are properly trained in the use of the system and that it functions correctly and is regularly maintained,” says Van der Elst. “Lasers, electrosurgical instruments, high-frequency echoes and the like all have their advantages, but they also all pose risks.”
“When you find yourself on such an operating table, you fully realise that you are surrendering yourself not only to doctors and nurses but also to all the equipment they use. You can only hope that the staff are properly trained in the use of the system and that it functions correctly and is regularly maintained,” says Van der Elst. “Lasers, electrosurgical instruments, high-frequency echoes and the like all have their advantages, but they also all pose risks.”
So how can we use smart technologies to make healthcare safer for patients? That is one of the questions Van der Elst will be addressing in the coming years. It is a question that poses quite a challenge. “Based on figures from abroad, we estimate that each year some six thousand patients in the Netherlands suffer serious damage as a result of a potentially preventable healthcare incident; 1500 of these die as a result. There are various causes of this: diagnostic or medication errors, infections, falls, but also technological failures.” So there is plenty of subject matter for research. The renowned ECRI Institute in the US publishes an annual top ten of technological risks in healthcare, ranging from loose bolts and screws to unproven robotic surgical techniques.
Patient values
However, safety is not the only important factor in the development and application of technology in healthcare. “Safety is very important, but other patient values also need to be explicitly taken into account when introducing new healthcare technologies,” says Van der Elst. “Patients want to keep a certain degree of autonomy, they want privacy and they want to be treated with dignity and compassion,” he gives as examples. “We can use technology to facilitate self-management of chronic conditions, help people to live at home for longer and improve their quality of life, which are all things that patients value.”
Nonetheless, this important issue is receiving too little attention at the moment. “New technologies in hospitals are currently very industry-driven. Moreover, the technologies that are promoted as the best solutions often also turn out to be the more expensive ones.” This is unsurprising if you consider the high development costs of medical technology, or MedTech, but according to Van der Elst this is putting the cart before the horse. “Some people even come to me and say: ‘Look what I’ve developed; do you have a patient for it?’ But that’s not the way it works. We should judge a new technology based on its value for the patient and the patient’s quality of life, and its usefulness for the professional. For example, does it make a surgical procedure less painful or easier to perform?”
But the interests of society must be taken into account too. “Healthcare costs make up a significant part of public expenditure, so you have to be able to justify that the money is being put to good use. Does the new technology really make treatment more efficient and cheaper?” For example, a Da Vinci surgical system costs €2.5 million. “To this, you can add thousands of euros per operation for the use of the sterile casings. So there has to be convincing evidence that such a robotic procedure is much better than an ordinary operation,” says Van der Elst. “Our chair will enable us to investigate the use of such new technologies or critically examine the evidence provided by others.”
The robotisation of healthcare will certainly not stop with the Da Vinci robot. Transferring tasks from hospital staff to robots can resolve a lot of the current challenges in healthcare, Van der Elst thinks. Stock management, for example, is a task that healthcare staff should not have to concern themselves with. “Logistics in supermarkets and Ikea stores are fully automated, so why does it all have to be done manually in a hospital? This work can all be done automatically using sensors.” Transferring such tasks to robots has another important advantage. “Staff get frustrated because they can only spend 60% of their time providing actual care. If technology can assume all those tedious administrative and stock management tasks, or make the beds, the nurses will have more time for the patients. And this will attract young people back to the healthcare sector.”
We can use technology to facilitate self-management of chronic conditions, help people to live at home for longer and improve their quality of life, which are all things that patients value.”

Roadmap
Van der Elst has a clear idea of what he wants to have achieved by the time he passes the baton to another clinician in five years’ time. “I will be satisfied if by that time there is a roadmap for every technological innovation in a hospital. This will enable us to ensure that we only introduce new technologies that have proven effective, that are more efficient and cheaper, and that take the interests and values of the patients into account. Then we’ll really have achieved something.”